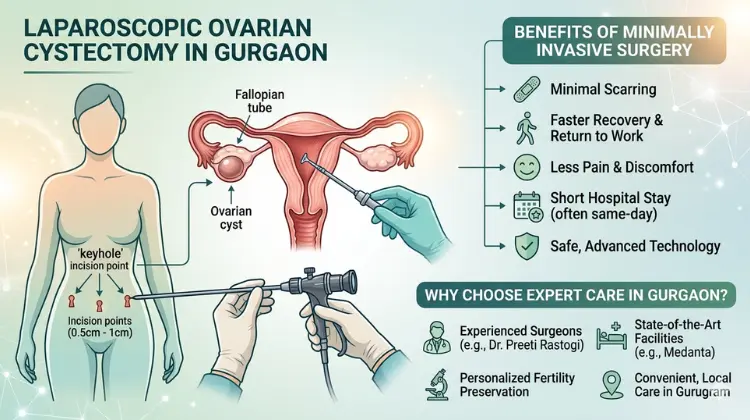
Comparing the Benefits: Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery
Managing your reproductive health often comes with tough decisions, especially when diagnosed with an ovarian cyst that requires surgical intervention. The primary choice usually boils down to Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery. While both procedures aim to remove the cyst and preserve ovarian function, they differ significantly in technique, recovery time, and long-term outcomes.
In this guide, we will break down the key differences to help you understand why many women and surgeons today prefer the minimally invasive approach.
What is Laparoscopic Ovarian Cystectomy?
A Laparoscopic Ovarian Cystectomy is a modern, minimally invasive procedure. Instead of one large incision, a surgeon makes 3–4 tiny incisions (usually 0.5 to 1 cm) in the abdomen. A laparoscope—a thin tube with a high-definition camera—is inserted, allowing the surgeon to view the pelvic organs on a monitor and remove the cyst with precision tools.
Key Advantages of the Laparoscopic Approach
-
Minimal Scarring: Because the incisions are tiny, they often require only a single stitch or surgical glue.
-
Faster Recovery: Most patients return to their normal routine within 1 to 2 weeks.
-
Reduced Pain: Less tissue trauma means significantly lower post-operative discomfort.
-
Shorter Hospital Stay: Many patients go home the same day or within 24 hours.
What is Traditional Open Surgery (Laparotomy)?
Traditional Open Surgery, also known as a laparotomy, involves a single large incision (typically 10–15 cm) across the lower abdomen. This method provides the surgeon with direct physical access and a wide field of view.
While laparoscopy is the gold standard for benign cysts, Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery comparisons often highlight that open surgery is still necessary for:
-
Extremely large cysts (typically over 10–15 cm).
-
Cases where there is a high suspicion of malignancy (cancer).
-
Complex internal adhesions from previous surgeries.
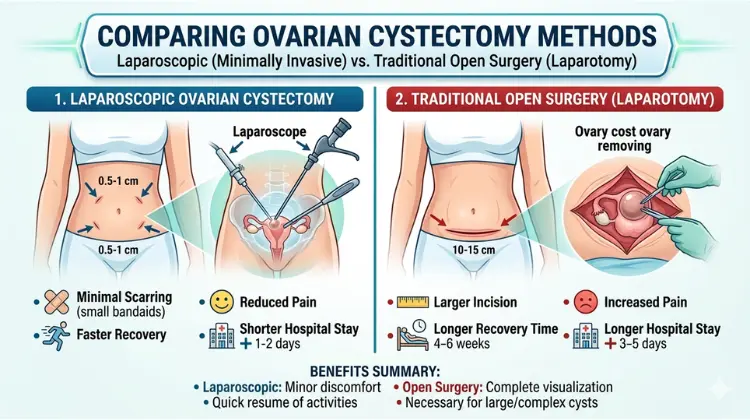
Comparing the Benefits: Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery
When evaluating Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery, it is essential to look at the clinical outcomes and the impact on your lifestyle.
1. Surgical Precision and Fertility
Laparoscopic surgery uses magnification, which helps surgeons peel the cyst wall away from healthy ovarian tissue more precisely. This is crucial for women of reproductive age who wish to preserve their fertility. In contrast, Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery studies suggest that open surgery may carry a slightly higher risk of forming internal adhesions (scar tissue) that can affect the fallopian tubes.
2. Infection and Complication Rates
Smaller incisions mean less exposure of internal organs to the air, which reduces the risk of post-operative infections. In the debate of Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery, laparoscopy consistently shows lower rates of blood loss and wound-related complications.
3. Recovery Timeline
-
Laparoscopic: Recovery takes 7–14 days.
-
Traditional Open: Recovery takes 4–6 weeks.
The choice between Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery often hinges on how quickly a patient needs to return to work or care for their family.
Also Read: Recovery Timeline: Returning to Work After Laparoscopic Ovarian Cystectomy in Gurgaon
Making the Right Choice
While the benefits of the minimally invasive route are clear, the “best” surgery is the one that is safest for your specific condition. During your consultation, your gynecologist will review your ultrasound or MRI results to decide if Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery is the right path for you.
For patients in urban hubs like Gurgaon, accessing advanced robotic or laparoscopic facilities is easier than ever. Choosing an experienced surgeon who specializes in these techniques ensures that the debate of Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery ends with the best possible health outcome for you.
The Expertise of Dr. Preeti Rastogi
With over 30 years of experience spanning India and the United Kingdom, Dr. Preeti Rastogi is a veteran in gynecological care and is widely recognized as the best gynecologist in Gurgaon for complex surgical interventions. Currently serving as the Director and HOD of Obstetrics and Gynaecology at Medanta – The Medicity, Gurgaon, she is among the elite group of surgeons in India certified to operate the Da Vinci Xi Robotic System, ensuring that the choice between Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery always results in the most advanced care possible. Her prestigious qualifications include an MRCOG from the Royal College of Obstetricians and Gynaecologists, London, and a specialized Fellowship in Urogynaecology from the UK, underscoring her commitment to global medical standards.
#OvarianCystRemoval #MinimallyInvasiveSurgery #LaparotomyVsLaparoscopy #GynecologicalSurgery #RecoveryAfterCystectomy #OvarianCystSymptoms #FertilityPreservation #PCOS #EndometriosisSurgery #GurgaonGynecologist #WomenHealth #SurgicalRecovery #LaparoscopicSurgeon #PelvicPain #CystectomyRisks #OvarianCystTreatment #BenignOvarianCyst #RoboticCystectomy #PostOpCare #HealthTips #GynecologyGurgaon #InfertilityTreatment #SmallIncisionSurgery #MedicalComparison #PainManagement #KeyholeSurgery #AbdominalSurgery #OvarianHealth #ExpertGynecologist #SurgicalSafety
Understanding the Surgical Differences
When evaluating your options, understanding the nuances of a laparotomy for ovarian cyst versus modern minimally invasive gynaecology is crucial for long-term health. The post-operative recovery varies significantly between the two; while traditional methods involve a large incision, laparoscopy focuses on reducing surgical scarring and pain. At the Medanta gynaecology department, patients often have access to robotic-assisted surgery, which is the gold standard for benign ovarian cyst removal. By adhering to global patient safety standards, surgeons ensure proper abdominal incision care and utilize laparoscopic precision to minimize trauma.
In complex cases involving gynaecological oncology, an infection risk comparison shows that smaller incisions significantly lower complications. Furthermore, the hospital stay duration is drastically reduced with “keyhole” techniques, which are also superior for pelvic adhesion prevention and ovarian tissue preservation. By leveraging advanced surgical technology, the debate of cystectomy vs oophorectomy is often resolved in favor of saving the organ. Minimizing blood loss in surgery helps patients suffering from chronic pelvic pain recover faster. Always seek an expert surgical consultation to determine which approach aligns with your specific medical needs.
Frequently Asked Questions
1. Is Laparoscopic Ovarian Cystectomy safer than Traditional Open Surgery?
Generally, yes. For benign cysts, laparoscopy is considered safer due to lower risks of infection, less blood loss, and fewer post-operative complications compared to open surgery.
2. How long is the hospital stay for Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery?
Laparoscopic patients are often discharged within 24 hours. Traditional open surgery usually requires a hospital stay of 2 to 4 days for monitoring.
3. Can large cysts be removed laparoscopically?
Yes, many skilled surgeons can remove cysts larger than 10cm using laparoscopy by “bagging” the cyst and draining it before removal. However, if cancer is suspected, open surgery is preferred.
4. How do I find the best gynecologist in Gurgaon for laparoscopic surgery?
Look for a gynecologist in Gurgaon who has specialized fellowship training in “Minimally Invasive Gynecology” or “Laparoscopic Surgery.” Check hospital affiliations (like Max or Fortis) and read patient reviews regarding their success with complex cyst removals.
5. What is the cost difference between Laparoscopic Ovarian Cystectomy vs. Traditional Open Surgery in Gurgaon?
Laparoscopic surgery may have a higher upfront cost due to specialized equipment, but it often proves more economical overall because of the shorter hospital stay and faster return to work.